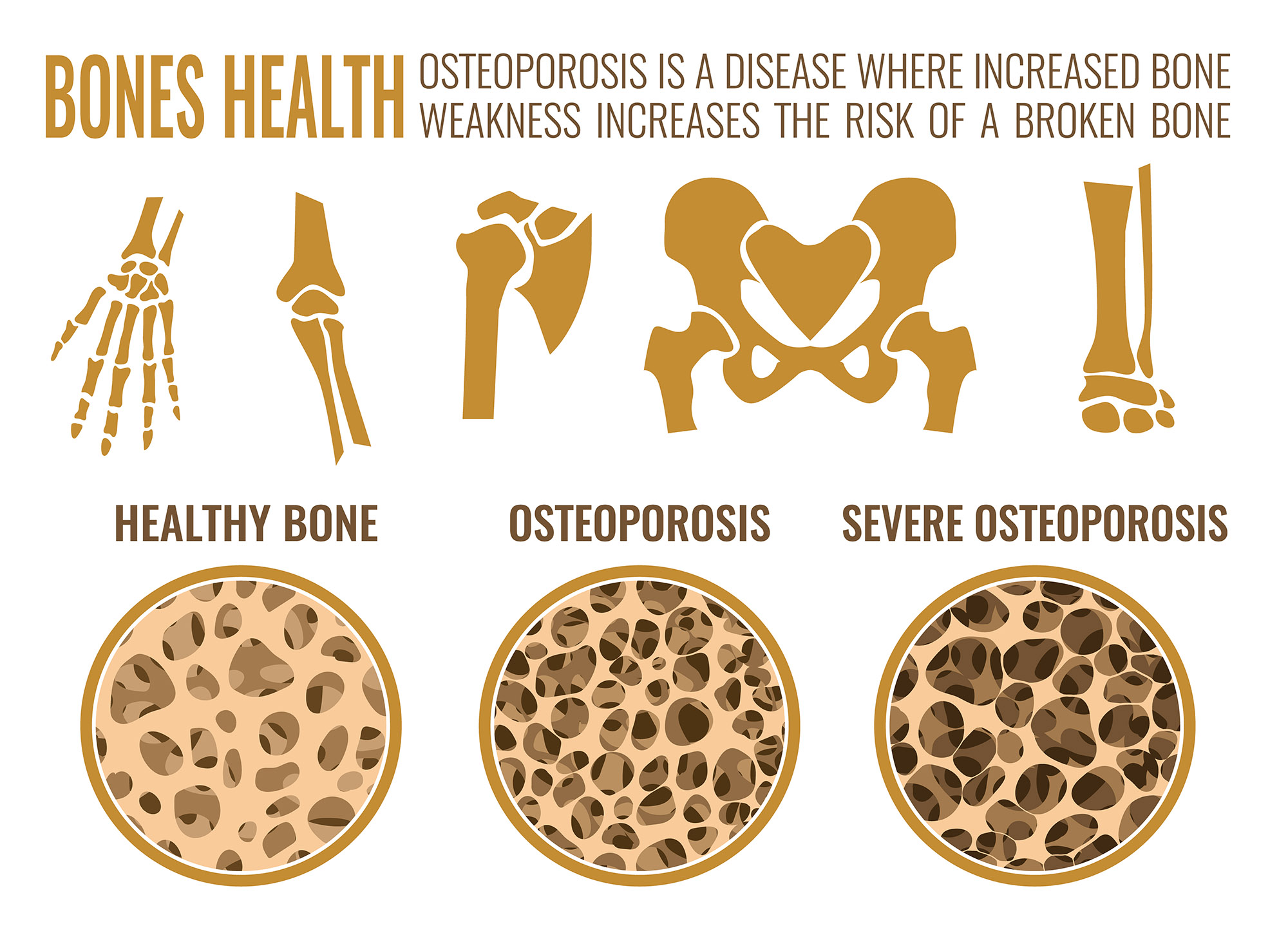
Osteoporosis is a condition that affects millions of people worldwide, characterized by a decrease in bone density and an increased risk of fractures. It is often associated with aging, particularly in postmenopausal women, but it can also affect men and younger individuals. One of the most pressing questions for those diagnosed with osteoporosis is: Can Osteoporosis Be Reversed? This blog post will delve into the complexities of osteoporosis, exploring the potential for reversal, and providing insights into effective management strategies.
Understanding Osteoporosis
Osteoporosis is a bone disease that occurs when the body loses too much bone, makes too little bone, or both. As a result, bones become weak and may break from a fall or, in serious cases, from sneezing or minor bumps. The condition is often referred to as a "silent disease" because it progresses without symptoms until a fracture occurs.
There are several types of osteoporosis, including:
- Primary Osteoporosis: This is the most common type and is often associated with aging and hormonal changes, particularly in postmenopausal women.
- Secondary Osteoporosis: This type is caused by other medical conditions or medications, such as long-term use of corticosteroids.
- Idiopathic Osteoporosis: This type occurs in younger individuals without a known cause.
Can Osteoporosis Be Reversed?
The question of whether osteoporosis can be reversed is complex. While it is not possible to completely reverse the bone loss that has already occurred, it is possible to slow down or even stop further bone loss and, in some cases, to build new bone. This is typically achieved through a combination of lifestyle changes, medications, and medical interventions.
Lifestyle Changes for Managing Osteoporosis
Lifestyle changes play a crucial role in managing osteoporosis and can significantly impact bone health. Key lifestyle modifications include:
- Diet and Nutrition: A balanced diet rich in calcium and vitamin D is essential for bone health. Foods high in calcium include dairy products, leafy green vegetables, and fortified plant-based milks. Vitamin D, which aids in calcium absorption, can be obtained from sunlight, fatty fish, and fortified foods.
- Exercise: Regular physical activity, particularly weight-bearing and resistance exercises, can help strengthen bones and muscles. Examples include walking, running, weightlifting, and yoga.
- Avoiding Risky Behaviors: Smoking and excessive alcohol consumption can weaken bones and increase the risk of fractures. Quitting smoking and limiting alcohol intake are important steps in managing osteoporosis.
- Fall Prevention: Taking measures to prevent falls, such as removing tripping hazards, installing grab bars in the bathroom, and wearing supportive footwear, can help reduce the risk of fractures.
Medical Interventions for Osteoporosis
In addition to lifestyle changes, medical interventions are often necessary to manage osteoporosis effectively. These interventions can help slow down bone loss and, in some cases, promote bone growth. Common medical treatments include:
- Bisphosphonates: These medications, such as alendronate and risedronate, are commonly prescribed to slow bone loss and reduce the risk of fractures. They work by inhibiting the activity of osteoclasts, the cells responsible for breaking down bone tissue.
- Selective Estrogen Receptor Modulators (SERMs): SERMs like raloxifene can help maintain bone density and reduce the risk of fractures in postmenopausal women. They mimic the effects of estrogen on bone tissue without the associated risks.
- Parathyroid Hormone (PTH) Analogues: Medications like teriparatide stimulate bone formation and can be used to treat severe osteoporosis. They are typically prescribed for a limited duration due to potential side effects.
- Denosumab: This monoclonal antibody works by inhibiting the activity of osteoclasts and is administered via injection every six months. It is effective in reducing the risk of fractures in postmenopausal women and men with osteoporosis.
Monitoring Bone Health
Regular monitoring of bone health is essential for managing osteoporosis effectively. Bone density tests, such as Dual-Energy X-ray Absorptiometry (DXA) scans, can measure bone mineral density and assess the risk of fractures. These tests are typically recommended for:
- Women aged 65 and older.
- Men aged 70 and older.
- Postmenopausal women under 65 with risk factors for osteoporosis.
- Men aged 50-69 with risk factors for osteoporosis.
- Individuals with a history of fractures or conditions that increase the risk of osteoporosis.
It is important to note that bone density tests should be repeated periodically to monitor changes in bone health and adjust treatment plans as needed.
📝 Note: Regular follow-ups with healthcare providers are crucial for effective management of osteoporosis. These visits allow for adjustments to treatment plans based on individual needs and responses to therapy.
Emerging Treatments and Research
Research into osteoporosis is ongoing, and new treatments are continually being developed. Some emerging therapies and areas of research include:
- Anabolic Agents: These medications stimulate bone formation and are being studied for their potential to reverse bone loss. Examples include abaloparatide and romosozumab.
- Bone Marrow Transplants: In some cases, bone marrow transplants have been used to treat severe osteoporosis by replacing damaged bone marrow with healthy cells.
- Gene Therapy: Researchers are exploring the use of gene therapy to correct genetic mutations that contribute to osteoporosis. This approach holds promise for treating inherited forms of the disease.
Support and Resources for Osteoporosis Management
Living with osteoporosis can be challenging, but there are numerous resources and support systems available to help individuals manage the condition effectively. These include:
- Support Groups: Joining a support group can provide emotional support, practical advice, and a sense of community. Many organizations offer local and online support groups for individuals with osteoporosis.
- Educational Resources: There are numerous books, websites, and online courses that provide information about osteoporosis, its management, and the latest research findings.
- Healthcare Providers: Working closely with healthcare providers, including primary care physicians, endocrinologists, and physical therapists, can help ensure that individuals receive the best possible care and support.
By leveraging these resources, individuals with osteoporosis can gain a better understanding of their condition and develop effective strategies for managing it.
📝 Note: It is important to consult with healthcare providers before making any significant changes to lifestyle or treatment plans. They can provide personalized advice and guidance based on individual needs and health status.
Osteoporosis is a complex condition that requires a multifaceted approach to management. While it is not possible to completely reverse the bone loss that has already occurred, it is possible to slow down or even stop further bone loss and, in some cases, to build new bone. By combining lifestyle changes, medical interventions, and regular monitoring, individuals with osteoporosis can improve their bone health and reduce the risk of fractures. Ongoing research and emerging treatments offer hope for even more effective management strategies in the future.
Related Terms:
- can osteoporosis be prevented
- can osteoporosis be cured
- can osteoarthritis be reversed
- treatment for osteoporosis
- how to reverse osteoporosis quickly